Course Information
Course Overview
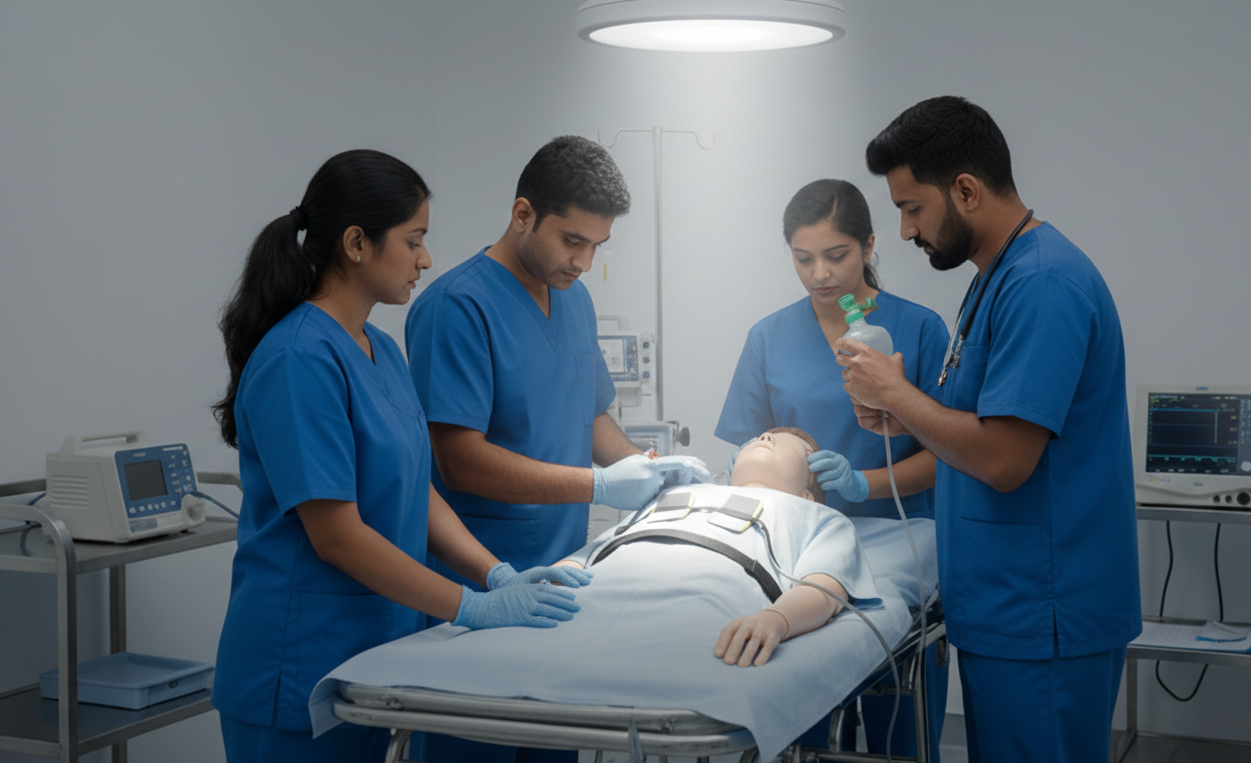
Master the essential skills to save lives with our American Heart Association (AHA) certified ACLS course. At RED TACT, we combine the global gold standard of AHA guidelines with our signature simulation-based training to ensure you are “code-ready” when every second counts.
Enrollment
Quick Facts
- Industry Recognized
- Expert Instructors
- Hands-on Training
- Lifetime Support
Who is this program for?
Designed for healthcare professionals requiring globally-recognized ACLS certification

Nurses
Physicians
Paramedics
Respiratory Therapists
Programme Highlights
Discover what makes our training programs exceptional
Globally Recognized AHA Certification
Advanced Pharmacology
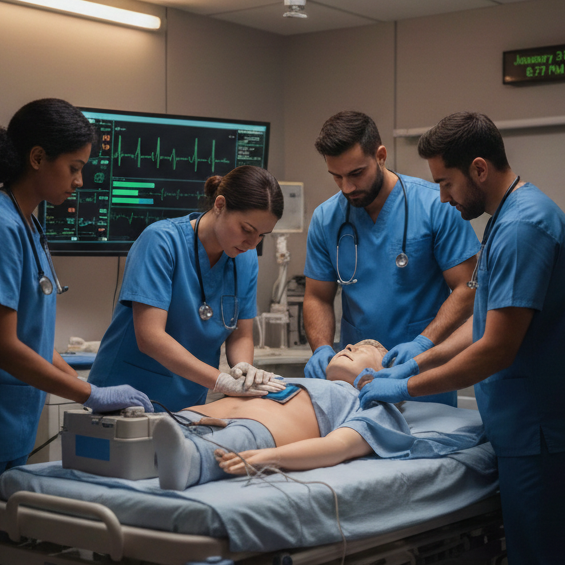
Simulation based learning
Certified Instructors
Curriculum & Specialisations
Our comprehensive training begins on Day 1 with Basic Life Support (BLS) in the morning, transitioning into Advanced Cardiovascular Life Support (ACLS) in the afternoon. Day 2 is dedicated to mastering remaining ACLS modules, followed by the final certification exam.
ACLS AlgorithmsrnAdvanced Cardiovascular Life Support (ACLS) moves beyond basic rescue to provide a systematic approach for treating life-threatening cardiovascular emergencies. This module teaches healthcare providers how to use standardized flowcharts to make rapid, evidence-based decisions during a crisis.rnrnKey areas of focus include:rnrnThe Adult Cardiac Arrest Algorithm: Mastering the branch-point decisions for shockable rhythms (VF/pVT) versus non-shockable rhythms (Asystole/PEA).rnrnBradycardia & Tachycardia Management: Identifying and treating symptomatic heart rates—whether too slow or too fast—using pharmacological interventions or electrical therapies like pacing and cardioversion.rnrnPost-Cardiac Arrest Care (ROSC): The critical steps to take once a pulse is regained to optimize neurological recovery and stabilize organ function.rnrnSpecialized Protocols: Rapid assessment and intervention pathways for Acute Coronary Syndrome (ACS) and Suspected Stroke to minimize long-term damage.rnrnH’s and T’s: Learning to troubleshoot and treat the reversible underlying causes of cardiac arrest, such as hypoxia, hypovolemia, and toxins.
Securing a patent airway is the first priority in any resuscitation effort. This module covers the essential skills and tools required to maintain oxygenation and ventilation, ranging from basic manual maneuvers to the use of advanced adjuncts.rnrnKey areas of focus include:rnrnManual Airway Maneuvers: Perfecting the Head-Tilt/Chin-Lift and the Jaw-Thrust (for suspected spinal injuries) to open the airway without equipment.rnrnOropharyngeal (OPA) & Nasopharyngeal (NPA) Airways: Determining when and how to use basic adjuncts to prevent the tongue from obstructing the throat.rnrnBag-Mask Ventilation (BVM): Mastering the E-C Clamp technique to ensure an airtight seal and effective lung inflation, whether working alone or in a team.rnrnAdvanced Airway Integration: Understanding the transition to advanced devices (like endotracheal tubes or supraglottic airways) and how to coordinate chest compressions without pausing for breaths.rnrnSuctioning & Clearing: Techniques for clearing fluids, vomit, or debris to prevent aspiration and maintain a clear path for oxygen.
In advanced resuscitation, the right medication at the right time can be the difference between life and death. This module focuses on the essential drugs used during ACLS and PALS, emphasizing dosages, administration routes, and the physiological "why" behind each choice.rnrnKey areas of focus include:rnrnVasopressors: Understanding the role of Epinephrine in increasing coronary and cerebral blood flow during cardiac arrest.rnrnAntiarrhythmics: Master the use of medications like Amiodarone and Lidocaine to stabilize heart rhythms in cases of refractory VF or pVT.rnrnSymptomatic Treatments: Protocols for using Atropine for bradycardia, as well as Adenosine for specific types of tachycardia.rnrnReversal & Supportive Agents: Identifying when to use specialized medications such as Magnesium Sulfate (for Torsades de Pointes) or Sodium Bicarbonate.rnrnAdministration Routes: Proper techniques for intravenous (IV) and intraosseous (IO) delivery, including the importance of a fluid flush to ensure the medication reaches the central circulation.
ECG/Rhythm InterpretationrnAccurate rhythm recognition is the vital bridge between assessment and action. This module transforms complex waveforms into actionable data, teaching students how to identify lethal arrhythmias and subtle cardiac changes with speed and confidence.rnrnKey areas of focus include:rnrnAnatomy of the ECG Strip: Understanding the electrical cycle of the heart, from the P-wave (atrial contraction) to the QRS complex (ventricular contraction) and the T-wave (repolarization).rnrnSystematic Interpretation: Learning a foolproof 5-step method to analyze any strip—evaluating rate, regularity, P-waves, PR interval, and QRS width.rnrnLethal Arrhythmia Recognition: Rapidly identifying "code-level" rhythms such as Ventricular Fibrillation (VF), Pulseless Ventricular Tachycardia (pVT), Asystole, and PEA.rnrnTachycardias & Bradycardias: Distinguishing between different types of heart blocks (First, Second, and Third-degree) and narrow- vs. wide-complex tachycardias (like SVT).rnrnClinical Correlation: Learning to treat the patient, not just the monitor—correlating ECG findings with physical symptoms like hypotension, altered mental status, or chest pain.
Resuscitation Team LeadershiprnA successful "code" requires more than just clinical skill; it requires a conductor. This module focuses on the "soft skills" of high-stakes medicine, training participants to manage the chaotic environment of a cardiac arrest through organized, clear, and confident leadership.rnrnKey areas of focus include:rnrnThe Team Leader Role: Understanding the "global view"—overseeing the entire resuscitation effort, ensuring high-quality CPR, and planning the next steps before they happen.rnrnClosed-Loop Communication: Mastering the technique of confirming orders to prevent medication errors and ensure tasks (like shocks or drug delivery) are completed accurately.rnrnClear Roles and Responsibilities: Learning how to assign specific tasks—compressor, airway, monitor, recorder—to team members based on their skill sets.rnrnConstructive Intervention: How to tactfully correct a team member’s technique (e.g., compression depth) or address a missed step in the algorithm without disrupting the flow of care.rnrnDebriefing and Review: Utilizing post-event analysis to identify successes and areas for improvement, fostering a culture of continuous clinical excellence.
Application Process
Simple and streamlined process
Course selection
Go through the program details to pick what
Payment process
Get a confirmation email
Get Started
Certificate
Earn a recognized certificate upon completion.
Student Testimonials
Hear from our successful graduates
Frequently Asked Questions
Find answers to common questions
No FAQs have been added yet. Please add FAQs through the course editor.
Ready to start your healthcare journey?
Schedule a call with our team for personalized guidance.